GLP-1 medications for persisting symptoms after concussion? One woman’s experiment (4/16/26 Newsletter)
This week, our lead article, GLP-1 medications for post-concussion syndrome? One woman’s experiment, is in the Therapies Under Research category.
Also in this newsletter:
Writers: Malayka Gormally, John Rosseel, Emily Sugg, and Zoe Marquis
Editors: Zoe Marquis and Malayka Gormally
Please Note: Going forward, we will be publishing the Concussion Update Newsletter once a month instead of twice a month to allow us to diversify our programming.
Do you find the Concussion Update helpful? If so, forward this to a friend and suggest they subscribe.
Opportunities
Tuesday, April 7, 6 pm ET: A free webinar, Dizziness after Concussion, presented by Dr. John Rutka and hosted by the Canadian Concussion Centre. Register in advance.
Thursday, April 16, 11 am PT: A free online session, “But You Look Great”: The Challenges of Living with an Invisible Injury, presented by Caren Sumption, CPC, CVA, CHW, hosted by Brain Northwest.
Friday, April 17, 7 am PT: A free webinar, Caregiver 2 Caregiver: Supporting Families of Young Children with Brain Injury/Concussions, presented by Berenice de la Cruz, PhD, hosted by The Center for Brain Injury Research and Training. Register in advance.
Tuesday, April 21, 6 pm ET: A free webinar, Anxiety, Depression & PTSD: Before and After Concussion, presented by Dr. Abe Snaiderman, hosted by the Canadian Concussion Centre. Register in advance.
Thursday, April 23, 12 – 2 pm ET: A free webinar, Domestic Violence and Brain Injury for Survivors and Caregivers, hosted by the Ohio Domestic Violence Network and Brain Injury Association of Ohio. Domestic violence, trauma, and its impact will be discussed, plus “trauma-informed care, domestic violence programs, brain injury support services, and forensic nursing, including how these services can help survivors heal, document injuries, and get the care they need.”
April deadline: Sign up for the next sessions of Love Your Brain Online yoga, mindfulness & education programs, which start in April. These six-week programs run in April, July, and October. Participants may choose between group discussion programs and yoga and discussion programs. There are also affinity group programs for caregivers, BIPOC, athletes, and other communities.
Applications open: Apply for a free, 5-day in-person community retreat for people with brain injury and caregivers, hosted by Love Your Brain.
A message from CEO Malayka Gormally
I’m honored to be the new CEO of Concussion Alliance, succeeding Conor Gormally, who will be pursuing a Master's degree. As a co-founder of Concussion Alliance, I bring to the organization my lived experience as a parent advocate as well as institutional continuity. I look forward to expanding our educational impact with patients, advocates, and healthcare providers. Please read my article about my journey with Concussion Alliance on the Women in Global Health website. I hope to connect with many of you in the upcoming year!
Therapies Under Research
GLP-1 medications for persisting symptoms after concussion? One woman’s experiment.
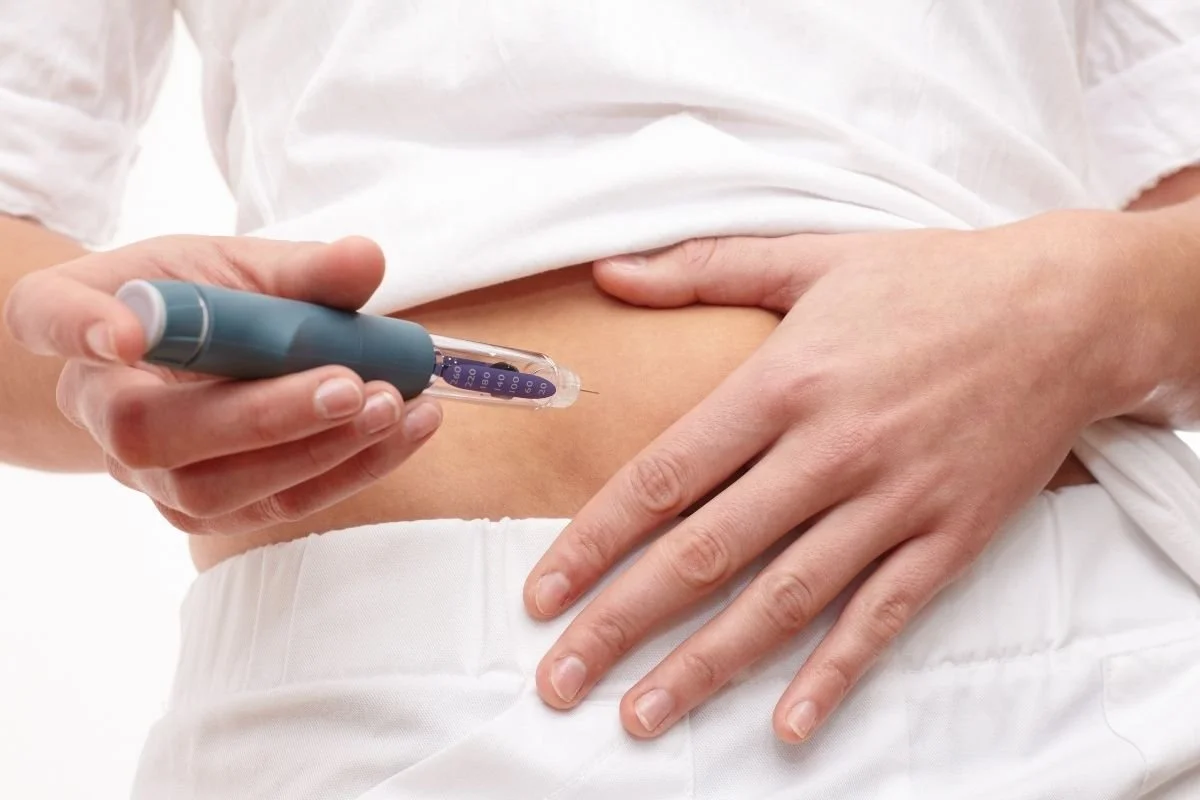
Both The Washington Post and The New York Times recently published articles about how GLP-1 medications (GLP-1s), approved for diabetes and weight loss, have a wider range of benefits for the body than previously thought, including potential benefits to the brain. There are downsides to the “Great American GLP-1 Experiment,” including serious side effects reported, the proliferation of GLP-1 prescribing by online telemedicine with “barriers to entry that are too low,” and the potential rebounding of health issues once the medication is stopped. However, along with these risks come some anecdotal stories of unusual benefits that warrant research. For example, The New York Times guest essay, by Julia Belluz, starts with an evocative story of a woman’s day-to-day experience with severe post-concussion syndrome, which had lasted ten years after she was hit by a car while on her bicycle. In 2025, Laurel Schmidt found a study on the neuroprotective effects of GLP-1s in cell and mouse models of mild traumatic brain injury (2016) and a review article on the therapeutic potential of GLP-1s in traumatic brain injury (2024). She contacted researchers, including chemist Richard DiMarchi at Indiana University, who suggested she ask her doctor if she could try GLP-1 “off-label” for her post-concussion syndrome. Schmidt started Zepbound and found her symptoms improved so significantly that she used the term “miraculous,” with her symptoms falling to a 6 out of 132 on the Post-Concussion Symptom Scale.
Dr. DiMarchi suspects that in Laurel Schmidt’s case, “the GLP-1 may have reduced damaging inflammation in her brain from her post-concussion syndrome,” and he thinks there should be clinical trials on GLP-1s for concussions. However, pharmaceutical companies may be reluctant to do clinical trials in areas such as traumatic brain injury, which are “difficult trials to run.” Public institutions such as the National Institutes of Health could play a role by funding research.
Note: While post-concussion syndrome (PCS) is the term many people still use, the new term used by researchers and clinicians is persisting symptoms after concussion (PSaC). The reason for the change is that each person who sustains a concussion will have a different combination of symptoms. In contrast, “syndrome” means a group of symptoms that always occur together.
The evidence is mixed regarding the neurological effects of GLP-1s. The Washington Post does not mention traumatic brain injury in its article that categorizes health conditions that are improved by GLP-s by level of evidence; Alzheimer’s and dementia are included in the “some evidence” category. Authors Ariana Eunjung Cha and Aaron Steckelberg refer to a Department of Veterans Affairs study, based on the data of 2.5 million patients, that found that “people prescribed GLP-1 drugs had a lower relative risk of developing dementia compared with those who took other drugs for diabetes.” Another study based on the medical records of over 100 million patients found that “Ozempic was linked to a lower risk of cognitive problems.” A study of liraglutide, an older GLP-1, found patients had slower cognitive decline than those not on the drug, and liraglutide “appeared to reduce shrinkage in key parts of the brain.” However, Novo Nordisk recently announced that its two clinical trials of semaglutide for dementia or mild cognitive impairment showed no cognitive benefits. The New York Times article stresses the urgent need for regulators and the medical establishment to keep pace with the experimentation that is happening with GLP-1s outside of research and clinical trials, and even outside the health system.
Statistics
Characteristics and symptoms of concussion in the ER that indicate increased likelihood of persisting symptoms at one month post-injury
A study by McIntosh et al. found that, for adults who presented with a concussion at the emergency department (ED) at a level 1 trauma center, certain characteristics and symptoms were significantly associated with an increased risk of persisting symptoms after concussion (PSaC) at one month post-injury. These characteristics and symptoms include female sex, post-traumatic amnesia, acute emotional or cognitive symptoms, and severe acute physical symptoms. Published in Neurology, the authors note that their study “uniquely contributes to the field by incorporating daily symptom tracking—a method not previously used in prognostic studies—to improve understanding of variables associated with time to recovery.” Female sex was a notable risk factor for PSaC; women took “twice as long to recover as men.” While only 50% of the participants were female, 70.6% of those with PSaC after 1 month were female. The presence of post-traumatic amnesia increased the odds of PSaC 5-fold, and also doubled recovery time. Acute, severe physical symptoms (headache, dizziness, neck pain, nausea, fatigue, etc) increased time to recovery by 8.4%. Acute emotional symptoms (irritability, sadness, anxiety) increased time to recovery by 5.5%. The authors advocate for emotional screening in the ED and referral for interventions such as cognitive behavioral therapy and other therapies, which research has shown to “reduce post-concussion symptoms, anxiety, and stress in adults with concussion.” For those with severe physical symptoms, the authors suggest symptom-specific treatments.
Recruited study participants were between the ages of 18 and 65, without evidence of intracranial abnormalities, and with no history of neurological disorder or prior moderate to severe TBI. These patients were evaluated by a healthcare professional after injury and discharged when deemed fit to leave. They were sent the Post-Concussion Symptom Checklist (PCSC) daily via text to evaluate their symptom progression with the focus on their recovery at the 1-month mark. This method allowed the researchers to track symptoms from day to day and determine the precise timing of symptom resolution. The researchers focused on specific characteristics identified in a previous systematic review and meta-analysis, including age, sex, post-traumatic amnesia, medical history, number of previous concussions, physical/cognitive/emotional symptoms, and sleep ability, all of which were self-reported. 150 participated in total with a 50/50 male-female divide.
McIntosh et al. acknowledge limitations in their sample size and their method of data collection. They emphasize the difficulty of using self-reported data, particularly about cognitive impairment. McIntosh et al. encourage further research using larger cohorts and a standardized health care tool to collect data and provide personalized care to each patient.
Education
A new, practical concussion guide for parents and coaches
The Archives of Physical Medicine and Rehabilitation has published a concussion recognition guide for parents and coaches that includes information on recognizing concussions and practical recovery advice. The authors, Dr. Ruairi Connolly and colleagues, based the guide on the 6th International Consensus Statement on Concussion in Sport (6th Consensus) and the American Congress of Rehabilitation Medicine (ACRM) definition of concussion/mild traumatic brain injury. The authors provide guidance on recognizing concussions, practical recovery advice, and general concussion knowledge to help parents and coaches be more prepared to handle concussions in their youth athletes. Below is a brief summary of the guide.
A sport-related concussion is a mild traumatic brain injury most often from a “direct blow to the head or body,” that transmits impulsive force to the brain, causing it to be “shaken inside the skull.”
A concussion can be identified, according to the ACRM, by one or more of the following clinical signs: if there is any loss of consciousness, trouble with memory or confusion (the child forgets where they are or is unable to remember who their coach is), or neurological symptoms such as headaches, dizziness, nausea, appearing dazed, or sensitivity to light or sound.
For a coach or parent, recognizing a concussion takes vigilance; some signs and symptoms occur immediately after injury, while some symptoms can take hours or up to three days to appear. The athlete may self-report symptoms like headaches, dizziness, trouble seeing, foggy vision, or feeling “slow” physically or mentally. Signs that may be observed immediately after a concussion include the athlete holding their head, stumbling or having trouble with balance, appearing dazed or confused, or being slow to answer questions.
It is good to keep checking in on the athlete as physical, cognitive, emotional, or sleep-related symptoms can develop up to 72 hours after the injury. Physical symptoms can include neck pain, headaches, nausea, vomiting, light and noise sensitivity, and blurred vision. Cognitive symptoms can include trouble concentrating, memory loss, or slowed thinking. Emotional symptoms can include nervousness, irritability, or sadness. Sleep-related symptoms can include sleeping more or less than is usual for the athlete, or even difficulty falling asleep.
The authors recommend the Concussion Recognition Tool 6 (CRT6) for identifying signs and symptoms of suspected concussion withinthe first 72 hours, according to the 6th consensus.
The best way to prevent long-term effects is to act promptly and cautiously. “If in doubt, sit them out,” is the golden rule for concussions. Continuing to play with a concussion can increase the risk of persisting symptoms after concussion, and cause more serious complications. Second-impact syndrome, though very rare, is a potentially life-threatening swelling of the brain that can occur when a second concussion happens before the brain has healed from the first concussion.
The first 24-48 hours after a concussion should involve physical and mental “relative rest.” Relative rest means that the athlete can do light activities of daily living, such as household tasks or going for a walk. They should reduce screentime and avoid challenging homework and intense exercise.
After the first 24-48 hours, the athlete should gradually increase physical activity; the guide recommends that this process be supervised by a health care professional (e.g., primary care physician, pediatrician, sports medicine specialist, or athletic trainer). Concerning return to play, the guide states “Never allows [sic] the athlete to return to play until evaluation by a health care professional experienced in concussion management has been completed.”
To clarify, Concussion Alliance notes that the 6th Consensus recommends medical clearance from a health care professional is required before the athlete progresses to activities that pose a risk of an inadvertent head impact (such as individual drills with a ball with teammates nearby), and after “full resolution of concussion symptoms.”
The guide recommends that, if symptoms last more than four weeks, patients should seek care from a concussion specialist. Concussion Alliance notes that the 6th Consensus recommends earlier rehabilitative care in some cases: the consensus recommends rehabilitative treatment for headaches, dizziness, and neck pain lasting more than 10 days.
Every athlete is different, and every recovery period is different. An athlete may fully recover in 2-4 weeks, but others may take longer. The authors suggest that “The best way to prevent the long-term effects of concussion is education, awareness, and prompt action.”
Diagnostics
The case for more intentional CT scan use in mTBI diagnosis
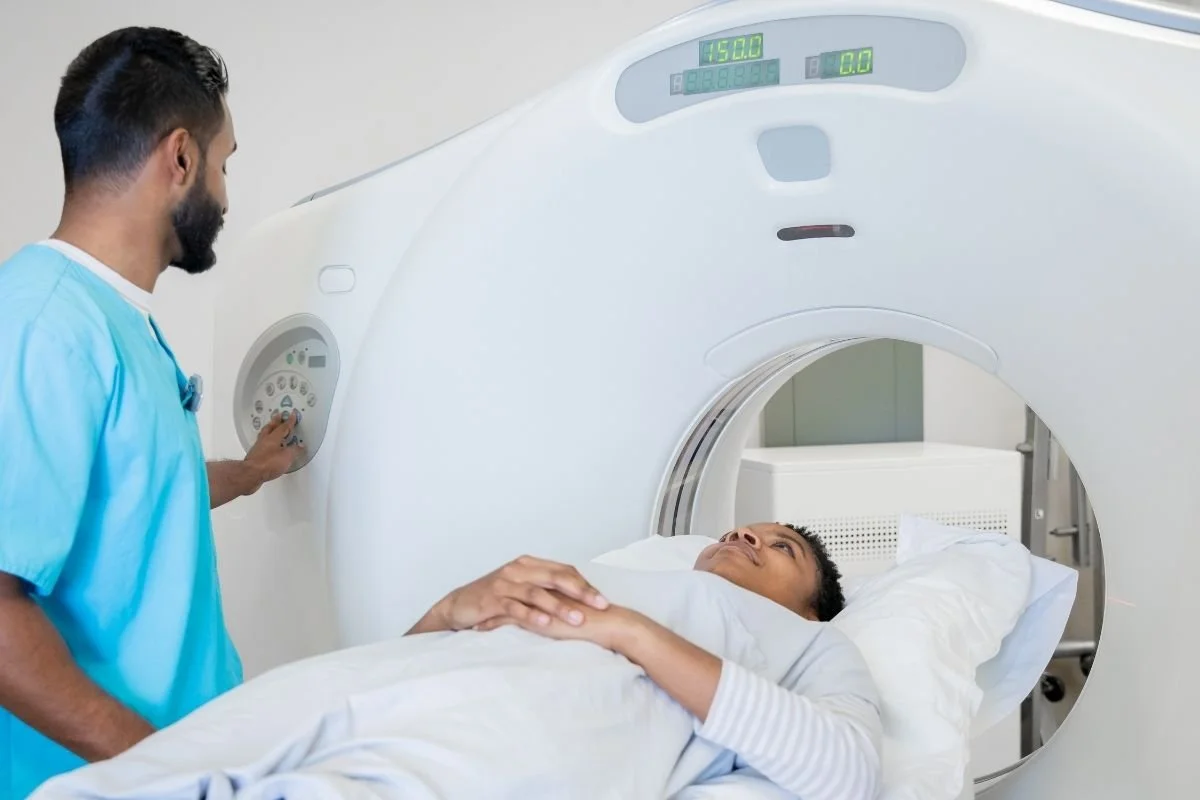
According to an editorial published in Cureus, computed tomography (CT) scans should be an available tool to support mild traumatic brain injury (mTBI) diagnosis, but should not be “the endpoint of thinking.” Currently, there are clinical decision rules, such as the Canadian CT Head Rule, that lay out criteria to help doctors determine when a CT scan is needed. However, the author, So Sakamoto, argues that misunderstanding and misapplication of these rules often lead to the overuse of CT scans without a meaningful improvement in outcomes. Sakamoto notes that “head CT is obtained in >80% of emergency department (ED) evaluations for suspected mTBI,” and CT scans can “quietly become the default response to anxiety: clinician anxiety, patient anxiety, and system anxiety.” To counteract this pattern, he proposes a practical approach: use imaging when it is likely to change injury management, ensure that decision rules are used within their intended limitations, and allow time for additional observation when immediate imaging is unlikely to change injury management. Sakamoto notes that this strategy requires systemic changes, such as supporting and prioritizing robust discharge planning and follow-up. Overall, moving away from rote rule application and towards more intentional use of CT scans within a broader diagnostic strategy can reduce unnecessary CT scanning and improve patient outcomes.
The Canadian CT Head Rule, Sakamoto notes, was created “to identify patients at risk of neurosurgical intervention and clinically important brain injury while safely reducing unnecessary CT use.” It was intended for patients with a “minor head injury” (Glasgow Coma Scale 13-15) who had a loss of consciousness (that was witnessed), amnesia, or disorientation. Misapplication of the rule means that clinicians may incorrectly rule out CT scan use for patients who do not meet those criteria (and thus were never eligible for the rule), or may put too much emphasis on a single criterion (such as age) and scan nearly everyone, even when scans are not necessary. For example, in a UK ED cohort of “fallers” (patients who have taken a fall) aged 65 years or older, 577 of 1172 received CT scans, but only 28 had an intracranial hemorrhage, and only two received neurosurgical intervention. These numbers are not to argue against imaging, but to show what imaging most often does—providing reassurance and stratifying risk more than triggering neurosurgical intervention.
Additionally, Sakamoto notes that in the original development of the Canadian CT Head Rule, patients with bleeding disorders and those using oral anticoagulants were excluded. However, Sakamoto contends that this does not mean patients in those categories must always undergo CT scans, but rather that the rule does not apply, and the decision requires clinician judgment. Thus, Sakamoto argues for a more intentional approach: using time, observation, and robust discharge planning, rather than immediate imaging. This approach, he argues, reduces unnecessary CT scanning while preserving safety.
You Can Support Concussion Patients
Join our community of monthly donors committed to improving how concussions are prevented, managed, and treated, thereby supporting long-term brain health for all. Learn more.
You can also make an impact with a one-time gift or tax-friendly options such as Donor Advised Funds (DAFs), IRA Charitable Rollovers, and Planned Giving: leave a gift in your will. Learn more.