Quick Guide: Navigating Your Concussion
Our downloadable quick guide, Navigating your Concussion, provides information on what to do if you suspect a concussion and how to manage your concussion recovery, whether you just experienced a concussion or it has been weeks or longer since you were injured.
The text for the quick guide is also on this page–scroll down.
This information reflects the most recent international guidelines in the 6th Consensus Statement on Concussion in Sport and The American Congress of Rehabilitation Medicine Diagnostic Criteria for Mild Traumatic Brain Injury. We also reference information from the Living Guideline for Pediatric Concussion from PedsConcussion and the CDC Heads Up resource.
Click here or on the images to download the PDF.
Below is the text from the quick guide:
If you suspect a concussion
A concussion is a mild traumatic brain injury that can occur when the head, neck, or body experiences a blow or jolt that transmits impulsive force to the brain, causing brain tissue to stretch, compress, and twist inside the skull.
Myths
Concussions only happen with:
a direct hit to the head
loss of consciousness
sports activities
See a healthcare provider
If you suspect a concussion, see a qualified medical provider within 24 - 48 hours: primary care, urgent care, or emergency department. (To read about when to call 911, scroll down to Red Flag Symptoms.)
Concussion symptoms
Following a blow or jolt to the head, neck, or body:
Dizziness or poor balance
headache
nausea
vision issues
difficulty remembering or concentrating
mental fog, confusion
neck pain/tenderness
sensitivity to light and noise
increased emotionality
Symptoms can appear up to 72 hours after injury.
Red Flag symptoms
Injury could be more severe; call 911 or go to the emergency department if you have:
Loss of consciousness
seizures/convulsions
slurred speech
severe increasing headache
weakness or tingling/burning in the arms or legs
being agitated/combative
one pupil being larger than the other
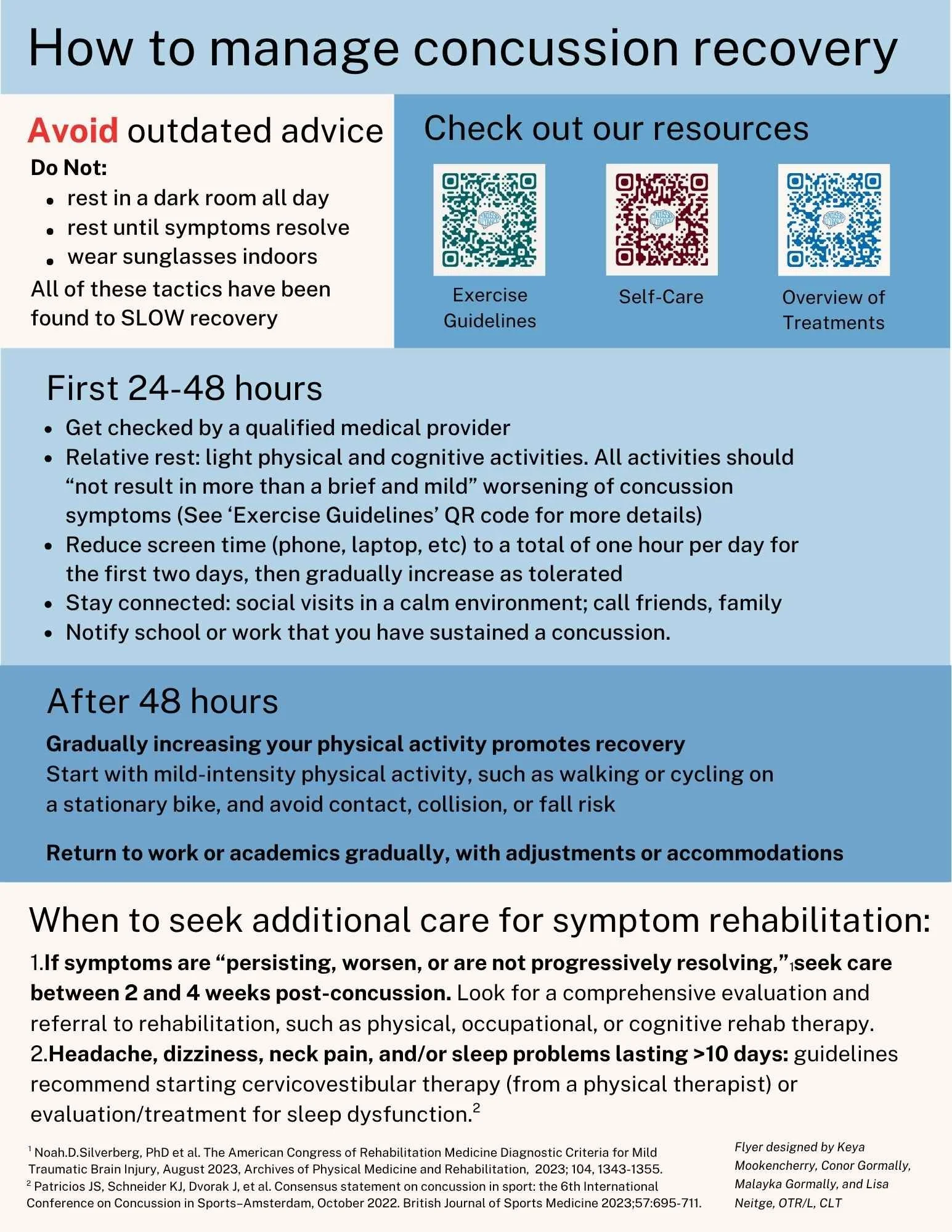
How to manage concussion recovery
Avoid outdated advice. Do not:
rest in a dark room all day
rest until symptoms resolve
wear sunglasses indoors
First 24-48 hours
Get checked by a qualified medical provider
Relative rest: light physical and cognitive activities. All activities should “not result in more than a brief and mild” worsening of concussion symptoms (See QR code for more details)
Reduce screen time (phone, laptop, etc) to a total of one hour per day for the first two days, then gradually increase as tolerated
Stay connected: visit friends in a calm environment; call friends, family
Notify school or work that you have sustained a concussion
After 48 hours
Gradually increasing your physical activity promotes recovery
Start with mild-intensity physical activity, such as walking or cycling on a stationary bike, and avoid contact, collision, or fall risk
Return to work or academics gradually, with adjustments or accommodations
When to seek additional care for symptom rehabilitation
1. If symptoms are “persisting, worsen, or are not progressively resolving,” seek care
between 2 and 4 weeks post-concussion. Look for a comprehensive evaluation and referral to rehabilitation, such as physical, occupational, or cognitive rehab therapy.
2. Headache, dizziness, neck pain, and/or sleep problems lasting >10 days: guidelines recommend starting cervicovestibular therapy (from a physical therapist) or evaluation/treatment for sleep dysfunction.
References:
1 Noah.D.Silverberg, PhD et al. The American Congress of Rehabilitation Medicine Diagnostic Criteria for Mild Traumatic Brain Injury, August 2023, Archives of Physical Medicine and Rehabilitation, 2023; 104, 1343-1355.
Patricios JS, Schneider KJ, Dvorak J, et al. Consensus statement on concussion in sport: the 6th International Conference on Concussion in Sports–Amsterdam, October 2022. British Journal of Sports Medicine 2023;57:695-711.
Quick guide created by Keya Mookencherry, Conor Gormally, Malayka Gormally, and Lisa Nietge, OTR/L, CLT